NICU SLP Salary and Job Outlook
Specializing in NICU speech-language pathology can be professionally and financially rewarding, though understanding the salary landscape requires looking at several factors: your geographic location, employment setting, and level of experience.
National Salary Benchmarks
According to the Bureau of Labor Statistics, the national median annual wage for speech-language pathologists was $95,410 in 2024, with a median hourly wage of $45.87.1 Hospital-based SLPs, the category that most closely reflects NICU clinicians, earned a median annual wage of $101,560, representing a meaningful premium over the overall SLP median.1 While there is no standalone BLS category for NICU SLPs specifically, hospital-based pediatric positions generally fall at or above that hospital median, particularly in large academic medical centers with Level III and Level IV NICUs. For a broader look at compensation across the profession, see our speech language pathologist salary breakdown.
Top-Paying States and Regional Variation
SLP salaries vary significantly by state, and these differences often reflect local cost of living as much as demand. A few standout states for SLP compensation include:
- California: Median annual wage of $116,000, the highest among states reporting, though housing and living costs significantly offset that figure.2
- Hawaii: Mean annual wage of approximately $107,040, again tempered by one of the nation's highest costs of living.3
- Other high-paying regions: States in the Northeast and Pacific Northwest also tend to report above-median SLP wages, driven by urban hospital systems and competitive labor markets.
When evaluating offers, look beyond the headline number. A $95,000 salary in a midsize Southern city may stretch further than $116,000 in coastal California.
Setting-Based Pay Differences
Your employment arrangement plays a large role in total compensation. Here is how the main settings compare for SLPs broadly, which provides useful context for NICU roles:
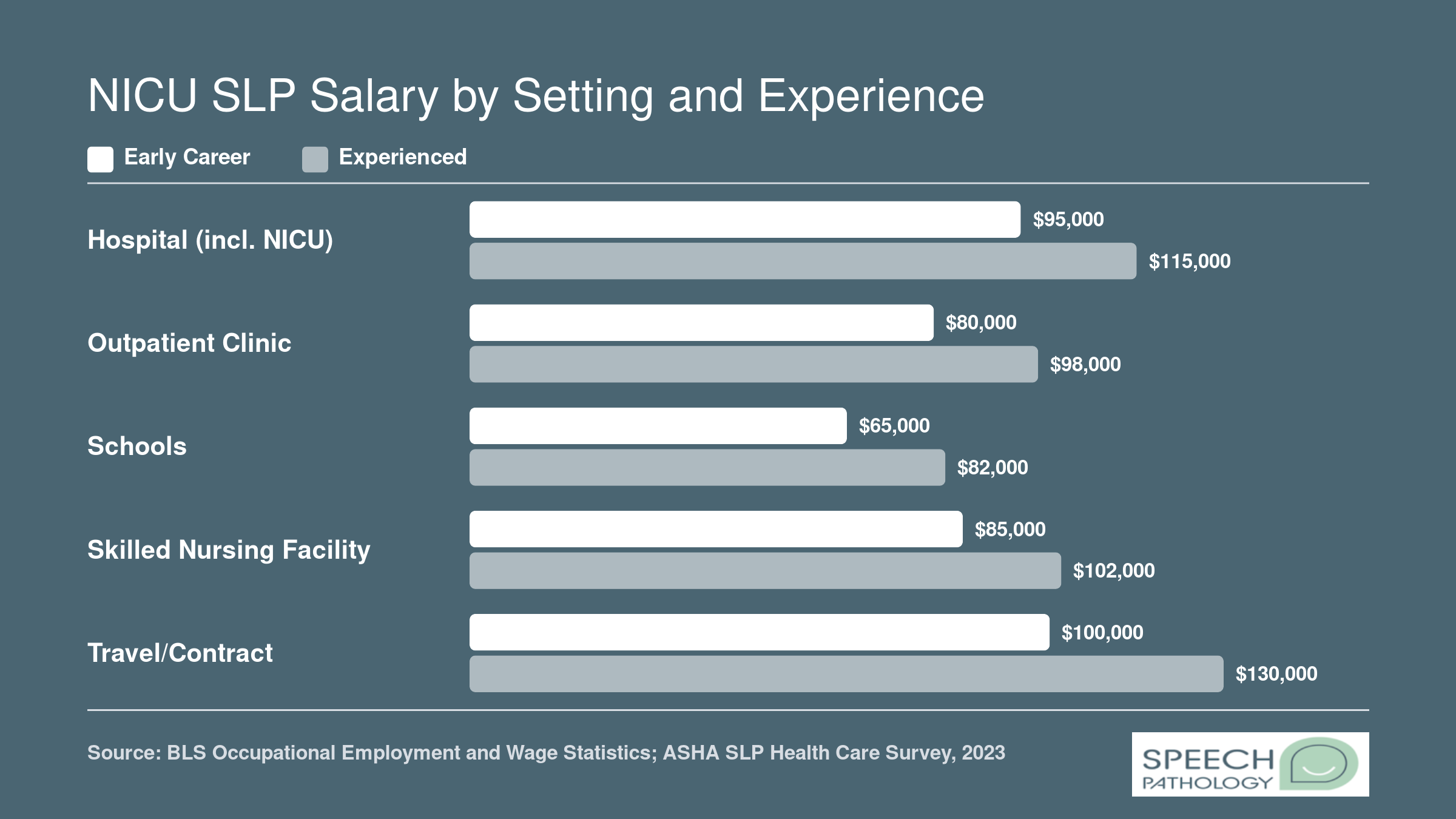
- Hospital-employed NICU SLPs: Stable salaries typically at or above the $101,560 hospital median, plus benefits packages including retirement plans, health insurance, and continuing education stipends.
- Travel or contract NICU positions: These roles often command higher hourly rates to compensate for the lack of benefits and job stability. Experienced NICU SLPs willing to travel can earn well above the national median, though these positions require adaptability and quick onboarding.
- Per-diem roles: Flexible but inconsistent. Per-diem NICU SLPs may earn competitive hourly pay without guaranteed hours or benefits.
For comparison across other SLP settings, school-based SLPs earned a median of $80,280, while SLPs in nursing and residential care facilities earned around $106,500.1 Home health care SLPs reported a median of $121,260, though that figure reflects a mix of specialties and caseload structures that differ substantially from hospital-based NICU work.1 When prospective SLPs ask what field pays the most, acute care hospital roles and home health tend to lead, with NICU positions falling squarely in the upper tier of hospital compensation.
Job Growth and Demand
The BLS projects 7% job growth for speech-language pathologists from 2024 to 2034, which is faster than the average for all occupations.4 Total employment stood at roughly 187,400 in 2024.4 NICU-specific positions represent a small fraction of that total because only hospitals with dedicated neonatal units employ these specialists. However, demand remains stable: premature birth rates in the United States have not declined, and growing awareness of early feeding intervention continues to reinforce the need for skilled NICU SLPs.
The limited number of openings means competition for NICU roles can be stiff, especially in desirable metro areas. Clinicians who pursue advanced neonatal training and build relationships with hospital systems during clinical fellowships or early career rotations position themselves most effectively. For more on the speech language pathology career outlook, explore our jobs guide.