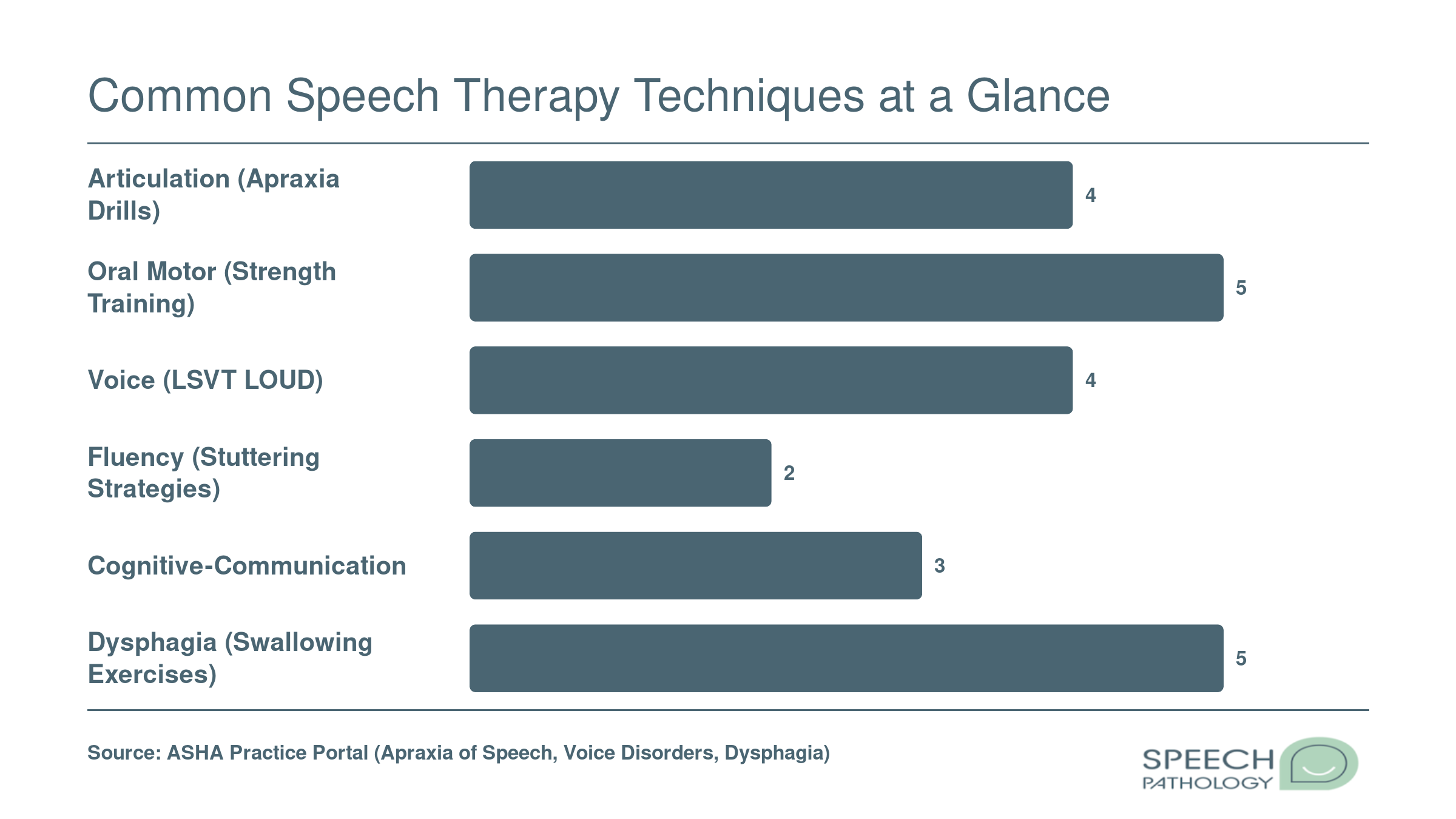
How SLPs Structure Sessions, Track Progress, and Adapt Exercises
Knowing which exercises exist is only half the equation. The other half is understanding how SLPs sequence those exercises within a session, measure change over time, and adjust intensity to match each patient's needs and energy level.
Anatomy of a Typical Session
Most speech therapy sessions follow a predictable arc that balances structured drill with real-world application:
- Warm-up drill: A brief, lower-demand activity that primes the target skill. For articulation, this might be isolated sound repetitions; for voice therapy, gentle humming or breath support exercises.
- Targeted exercise block: The core of the session, where the SLP works on specific goals at an appropriate challenge level. This block consumes the largest share of session time and often involves multiple repetitions or trials to build motor memory or linguistic accuracy.
- Functional carryover activity: A structured conversation, storytelling task, or role-play scenario that encourages the patient to use the target skill in a more natural context.
- Home practice assignment: The SLP reviews what the patient (or caregiver) should practice between sessions, including how many repetitions, which cues to use, and what to track.
Session length typically ranges from 30 to 60 minutes depending on the clinical setting and diagnosis. Acute care or inpatient rehab sessions may run shorter due to patient fatigue, while outpatient and school-based sessions often fill a full 30- or 45-minute slot.
Tracking Progress With Probe Data and Benchmarks
SLPs rely on structured probe data to measure whether an exercise is working. At regular intervals, often at the start of a session before practice effects kick in, the clinician records percent accuracy across a set of trials. A common advancement benchmark is 80 percent accuracy across three consecutive sessions at a given level before the difficulty increases. This data-driven approach keeps therapy moving forward without pushing a patient past readiness. Clinicians who want a deeper look at formal testing options can review our guide to speech language pathology assessment tools.
Beyond session probes, SLPs schedule standardized re-assessments at intervals dictated by the setting and payer requirements. These formal checkpoints compare current performance against baseline scores and inform whether goals need revision.
Technology and App Integrations
Digital tools have become a practical extension of the therapy room, giving patients structured practice on days they do not see their clinician. Several platforms stand out for their clinical utility:
- Constant Therapy: Designed for adults recovering from stroke or brain injury, this app offers exercises targeting language, cognition, and speech. It uses adaptive algorithms to adjust difficulty based on performance and provides a clinician dashboard so the SLP can monitor home practice remotely.
- Tactus Therapy: A suite of apps for aphasia, apraxia, and cognitive-communication disorders. Clinicians can customize which activities a patient accesses and review usage data between sessions.
- Speech Blubs: Aimed at pediatric populations, this app uses video modeling from real children to encourage sound and word production in younger learners.
These tools do not replace direct therapy, but they help bridge the gap between sessions by adding structured repetitions that reinforce in-clinic gains. For a broader comparison of platforms across age groups, see our roundup of the best speech therapy apps.
Frequency, Intensity, and Adjusting for the Whole Patient
ASHA does not mandate a universal treatment schedule, but the evidence base offers useful guidance. Motor speech disorders such as apraxia of speech respond well to higher-intensity practice, often three to five sessions per week, especially in the early stages of recovery. Voice therapy protocols like Vocal Function Exercises typically call for daily home practice to build the endurance and coordination that carry over into conversation.
SLPs rarely work with a single diagnosis in isolation. Patients with traumatic brain injury may experience significant cognitive fatigue that limits session length and home practice tolerance. Individuals with progressive conditions like dementia may benefit more from compensatory strategies than from drill-heavy repetition. Skilled clinicians adjust frequency, session duration, and exercise complexity to account for these realities rather than following a one-size-fits-all dosage.
Group Versus Individual Therapy
Both formats have a role in a comprehensive treatment plan. Individual sessions allow the SLP to customize drill intensity, provide immediate corrective feedback, and target very specific goals. Group sessions, on the other hand, introduce peer modeling, social reinforcement, and conversational dynamics that are difficult to replicate one-on-one.
Group therapy is especially valuable for fluency disorders, where participants practice techniques in front of supportive listeners, and for aphasia, where structured group conversation builds confidence and communication effectiveness. The trade-off is reduced individualized attention, so many SLPs combine both formats when caseload and scheduling allow.
For students preparing to enter the field, understanding session structure and progress monitoring is just as important as memorizing exercise protocols. The exercises are the tools; knowing how to organize, measure, and adapt them is what turns a collection of techniques into effective therapy.